What Is the Regenexx®-SD?
Regenexx®-SD is bone marrow concentrate, which contains stem cells, the repair cells our body uses to replace injured or old cells. As we age or have big injuries, we may not be able to recruit enough of these cells to the site to fully repair the area. Bone marrow concentrate therapy is a way to restore your body’s joint and tendon function and reduce pain and inflammation. This type of treatment is often referred to as a BMAC procedure (bone marrow concentrate procedure).

When Is a Regenexx®-SD Bone Marrow Concentrate (BMAC) Procedure Performed?
The goal of the procedure is to reduce pain and improve function by promoting the body’s own ability to heal naturally. This patented bone marrow concentrate protocol can be used for a wide range of orthopedic conditions. If your condition is causing you chronic pain and inflammation and negatively impacting your way of life, we may recommend bone marrow concentrate therapy to provide you with the relief you need.
How Is a Regenexx®-SD Bone Marrow Concentrate Procedure Performed?
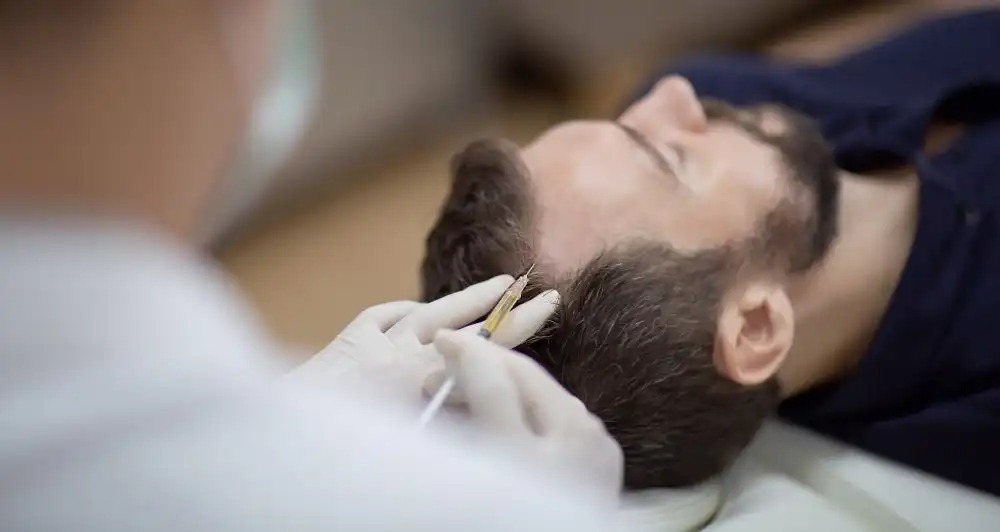
The Regenexx®-SD Procedure involves harvesting bone marrow from an area of the back of the hip that contains a dense population of stem cells and then concentrating those cells before precisely injecting them into the injured area using advanced imaging guidance.
How Do I know If Bone Marrow Concentrate Is an Appropriate Option for Me?
You may be an ideal candidate for bone marrow concentrate therapy if you’re living with osteoarthritis or another joint condition that’s preventing you from performing daily activities, hobbies, and more. Dr. Santo will evaluate your condition and your imaging to determine whether a bone marrow concentrate or platelet-based treatment is the best option for your orthopedic condition. We’re committed to restoring your quality of life, so you can get back to doing what you love without suffering from inflammation. Contact us to find out about bone marrow concentrate therapy near me. If you’re considering a BMAC procedure, Dr. Santo will review your goals, medical history, and imaging to determine whether this approach is appropriate.

Frequently Asked Questions on Bone Marrow Derived Stem Cell Therapy to Treat Orthopedic Conditions
Both PRP and BMAC are regenerative orthopedic treatments derived from the patient’s own blood or marrow, but they differ in composition and potency. PRP is drawn from a blood sample and is rich in growth factors and platelets, which stimulate healing. BMAC contains not only growth factors but also actual stem cells capable of differentiating into cartilage and other tissues, as well as a broader array of regenerative cytokines. BMAC is generally considered a more potent — and more expensive — option. PRP is often used for earlier-stage or softer-tissue conditions, while BMAC may be preferred for more significant cartilage loss or structural damage.